Abstract
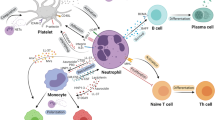
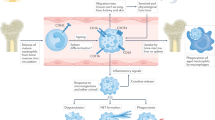
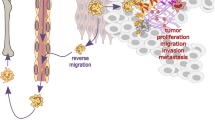
Recent studies have highlighted the functional capacity of neutrophils as powerful mediators of tissue inflammation. Granule-packaged proteases and reactive oxygen intermediates, which are important for intracellular digestion during phagocytosis, are released from neutrophils during inflammation. In the extracellular environment, neutrophil-derived proteases can cause local tissue damage, but also regulate the activity of cytokines, cytokine receptors and chemokines. Neutrophils can themselves produce an array of inflammatory mediators, including cytokines, chemokines and complement; these cells also express Fc receptors, which can bind and possibly transport immune complexes into the extravascular compartment, as well as activating neutrophils at opsonised surfaces. Blood-borne neutrophils interact with, and then exit through, the endothelium of blood vessels, after which these cells die and must be removed safely. The balance between neutrophil survival and clearance is crucial to the resolution of inflammation. A major regulator of neutrophil production and survival is the cytokine granulocyte colony-stimulating factor (G-CSF). Treatment with G-CSF can exacerbate underlying inflammatory diseases in humans and mice, and G-CSF deficiency is profoundly protective against collagen-induced arthritis in mice. These findings implicate G-CSF as an important proinflammatory cytokine. This article discusses the roles of neutrophils and G-CSF during chronic inflammatory diseases.
Key Points
-
There is extensive tissue infiltration by activated neutrophils in many inflammatory diseases
-
In addition to causing direct tissue damage, activated neutrophils can modulate inflammation via the local production or activation of cytokines, chemokines and complement
-
Neutrophils can be both targets and mediators of autoimmunity
-
Neutrophil apoptosis and clearance is essential for the resolution of inflammation
-
Granulocyte colony-stimulating factor, a key regulator of neutrophil production and survival, can have proinflammatory effects during inflammatory diseases such as rheumatoid arthritis
-
Inhibition of granulocyte colony-stimulating factor might provide a new therapeutic strategy in rheumatoid arthritis and other inflammatory diseases
-
The availability of granulocyte colony-stimulating factor means that, unlike other cytokine antagonists, it could be used to reverse inhibition of granulocyte colony-stimulating factor, if required
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Weiss SJ (1989) Tissue destruction by neutrophils. N Engl J Med 320: 365–376
Faurschou M and Borregaard N (2003) Neutrophil granules and secretory vesicles in inflammation. Microbes Infect 5: 1317–1327
Klebanoff SJ (2005) Myeloperoxidase: friend and foe. J Leukoc Biol 77: 598–625
Cassatella MA (1995) The production of cytokines by polymorphonuclear neutrophils. Immunol Today 16: 21–26
Scapini P et al. (2000) The neutrophil as a cellular source of chemokines. Immunol Rev 177: 195–203
de Oca RM et al. (2000) Polymorphonuclear neutrophils are necessary for the recruitment of CD8(+) T cells in the liver in a pregnant mouse model of Chlamydophila abortus (Chlamydia psittaci serotype 1) infection. Infect Immun 68: 1746–1751
McColl SR et al. (1998) Treatment with anti-granulocyte antibodies inhibits the effector phase of experimental autoimmune encephalomyelitis. J Immunol 161: 6421–3426
Bonder CS et al. (2004) Essential role for neutrophil recruitment to the liver in concanavalin A-induced hepatitis. J Immunol 172: 45–53
Scapini P et al. (2003) G-CSF-stimulated neutrophils are a prominent source of functional BLyS. J Exp Med 197: 297–302
Mackay F and Browning JL (2002) BAFF: a fundamental survival factor for B cells. Nat Rev Immunol 2: 465–475
Foell D and Roth J (2004) Proinflammatory S100 proteins in arthritis and autoimmune disease. Arthritis Rheum 50: 3762–3771
Pham CT (2006) Neutrophil serine proteases: specific regulators of inflammation. Nat Rev Immunol 6: 541–550
Adkison AM et al. (2002) Dipeptidyl peptidase I activates neutrophil-derived serine proteases and regulates the development of acute experimental arthritis. J Clin Invest 109: 363–371
Hu Y and Pham CT (2005) Dipeptidyl peptidase I regulates the development of collagen-induced arthritis. Arthritis Rheum 52: 2553–2558
Girardi G et al. (2003) Complement C5a receptors and neutrophils mediate fetal injury in the antiphospholipid syndrome. J Clin Invest 112: 1644–1654
Botto M et al. (1992) Biosynthesis and secretion of complement component (C3) by activated human polymorphonuclear leukocytes. J Immunol 149: 1348–1355
Hogasen AK et al. (1995) Human polymorphonuclear leukocytes store large amounts of terminal complement components C7 and C6, which may be released on stimulation. J Immunol 154: 4734–4740
Wipke BT et al. (2004) Staging the initiation of autoantibody-induced arthritis: a critical role for immune complexes. J Immunol 172: 7694–7702
Akgul C et al. (2001) Molecular control of neutrophil apoptosis. FEBS Lett 487: 318–322
Savill J et al. (2002) A blast from the past: clearance of apoptotic cells regulates immune responses. Nat Rev Immunol 2: 965–975
Lawrence T et al. (2002) Anti-inflammatory lipid mediators and insights into the resolution of inflammation. Nat Rev Immunol 2: 787–795
Hart SP et al. (2004) Immune complexes bind preferentially to Fc gamma RIIA (CD32) on apoptotic neutrophils, leading to augmented phagocytosis by macrophages and release of proinflammatory cytokines. J Immunol 172: 1882–1887
Sabroe I et al. (2003) Selective roles for Toll-like receptor (TLR)2 and TLR4 in the regulation of neutrophil activation and life span. J Immunol 170: 5268–5275
Jonsson H et al. (2005) Inflammatory arthritis requires Foxo3a to prevent Fas ligand-induced neutrophil apoptosis. Nat Med 11: 666–671
Dibbert B et al. (1999) Cytokine-mediated Bax deficiency and consequent delayed neutrophil apoptosis: a general mechanism to accumulate effector cells in inflammation. Proc Natl Acad Sci USA 96: 13330–13335
Liu-Bryan R and Terkeltaub R (2006) Evil humors take their toll as innate immunity makes gouty joints TREM-ble. Arthritis Rheum 54: 383–386
Inohara et al. (2005) NOD-LRR proteins: role in host-microbial interactions and inflammatory disease. Annu Rev Biochem 74: 355–383
Seo P and Stone JH (2004) The antineutrophil cytoplasmic antibody-associated vasculitides. Am J Med 117: 39–50
Xiao H et al. (2002) Antineutrophil cytoplasmic autoantibodies specific for myeloperoxidase cause glomerulonephritis and vasculitis in mice. J Clin Invest 110: 955–963
Xiao H et al. (2005) The role of neutrophils in the induction of glomerulonephritis by anti-myeloperoxidase antibodies. Am J Pathol 167: 39–45
van Boekel MA et al. (2002) Autoantibody systems in rheumatoid arthritis: specificity, sensitivity and diagnostic value. Arthritis Res 4: 87–93
Vossenaar ER et al. (2003) Citrullination of synovial proteins in murine models of rheumatoid arthritis. Arthritis Rheum 48: 2489–2500
Schimmer RC et al. (1997) Streptococcal cell wall-induced arthritis. Requirements for neutrophils, P-selectin, intercellular adhesion molecule-1, and macrophage-inflammatory protein-2. J Immunol 159: 4103–4108
Wipke BT and Allen PM (2001) Essential role of neutrophils in the initiation and progression of a murine model of rheumatoid arthritis. J Immunol 167: 1601–1608
Nandakumar KS et al. (2003) Collagen type II-specific monoclonal antibody-induced arthritis in mice: description of the disease and the influence of age, sex, and genes. Am J Pathol 163: 1827–1837
Kakimoto K et al. (1995) Suppressive effect of a neutrophil elastase inhibitor on the development of collagen-induced arthritis. Cell Immunol 165: 26–32
Halloran MM et al. (1999) The role of an epithelial neutrophil-activating peptide-78-like protein in rat adjuvant-induced arthritis. J Immunol 162: 7492–7500
Schrijver G et al. (1990) Anti-GBM nephritis in the mouse: role of granulocytes in the heterologous phase. Kidney Int 38: 86–95
Kelly KJ et al. (1996) Intercellular adhesion molecule-1-deficient mice are protected against ischemic renal injury. J Clin Invest 97: 1056–1063
Hellmich B et al. (2002) Autoantibodies against granulocyte colony-stimulating factor in Felty's syndrome and neutropenic systemic lupus erythematosus. Arthritis Rheum 46: 2384–2391
Campion G et al. (1990) The Felty syndrome: a case-matched study of clinical manifestations and outcome, serologic features, and immunogenetic associations. Medicine (Baltimore) 69: 69–80
Sanmarti R et al. (2005) Adsorptive granulocyte/monocyte apheresis for the treatment of refractory rheumatoid arthritis: an open pilot multicentre trial. Rheumatology (Oxford) 44: 1140–1144
Burgess AW and Metcalf D (1980) Characterization of a serum factor stimulating the differentiation of myelomonocytic leukemic cells. Int J Cancer 26: 647–654
Nicola NA et al. (1983) Purification of a factor inducing differentiation in murine myelomonocytic leukemia cells. Identification as granulocyte colony-stimulating factor. J Biol Chem 258: 9017–9023
Watari K et al. (1989) Serum granulocyte colony-stimulating factor levels in healthy volunteers and patients with various disorders as estimated by enzyme immunoassay. Blood 73: 117–122
Kaushansky K (2006) Lineage-specific hematopoietic growth factors. N Engl J Med 354: 2034–2045
Nicola NA and Metcalf D (1985) Binding of 125I-labeled granulocyte colony-stimulating factor to normal murine hemopoietic cells. J Cell Physiol 124: 313–321
Shimoda K et al. (1993) Identification of a functional receptor for granulocyte colony-stimulating factor on platelets. J Clin Invest 91: 1310–1313
Morikawa K et al. (2002) Characterization of granulocyte colony-stimulating factor receptor expressed on human lymphocytes. Br J Haematol 118: 296–304
Roberts AW (2005) G-CSF: a key regulator of neutrophil production, but that's not all! Growth Factors 23: 33–41
Croker BA et al. (2004) SOCS3 is a critical physiological negative regulator of G-CSF signaling and emergency granulopoiesis. Immunity 20: 153–165
Wong PK et al. (2006) SOCS-3 negatively regulates innate and adaptive immune mechanisms in acute IL-1-dependent inflammatory arthritis. J Clin Invest 116: 1571–1581
Basu S et al. (2002) G-CSF: function and modes of action (Review). Int J Mol Med 10: 3–10
Liu F et al. (1996) Impaired production and increased apoptosis of neutrophils in granulocyte colony-stimulating factor receptor-deficient mice. Immunity 5: 491–501
Lieschke GJ et al. (1994) Mice lacking granulocyte colony-stimulating factor have chronic neutropenia, granulocyte and macrophage progenitor cell deficiency, and impaired neutrophil mobilization. Blood 84: 1737–1746
Baumann R et al. (2004) Functional expression of CD134 by neutrophils. Eur J Immunol 34: 2268–2275
Chakraborty A et al. (2003) Granulocyte colony-stimulating factor promotes adhesion of neutrophils. Am J Physiol Cell Physiol 284: C103–C110
Rutella S et al. (2005) Granulocyte colony-stimulating factor: a novel mediator of T cell tolerance. J Immunol 175: 7085–7091
Brendolan A et al. (2003) Treatment of adjuvant arthritis with granulocyte-colony stimulating factor and peptide derived from heat shock protein 65. Cell Immunol 221: 6–14
Schots R et al. (1995) G-CSF in Felty's syndrome: correction of neutropenia and effects on cytokine release. Clin Rheumatol 14: 116–118
Snowden JA et al. (1998) A randomised, blinded, placebo-controlled, dose escalation study of the tolerability and efficacy of filgrastim for haemopoietic stem cell mobilisation in patients with severe active rheumatoid arthritis. Bone Marrow Transplant 22: 1035–1041
Moore J et al. (2002) A pilot randomized trial comparing CD34-selected versus unmanipulated hemopoietic stem cell transplantation for severe, refractory rheumatoid arthritis. Arthritis Rheum 46: 2301–2309
Campbell IK et al. (2000) The colony-stimulating factors and collagen-induced arthritis: exacerbation of disease by M-CSF and G-CSF and requirement for endogenous M-CSF. J Leukoc Biol 68: 144–150
Miyahara H et al. (1993) The effects of recombinant human granulocyte colony-stimulating factor on passive collagen-induced arthritis transferred with anti-type II collagen antibody. Clin Immunol Immunopathol 69: 69–76
Nakamura H et al. (2000) High serum and synovial fluid granulocyte colony stimulating factor (G-CSF) concentrations in patients with rheumatoid arthritis. Clin Exp Rheumatol 18: 713–718
Campbell IK et al. (1991) Human articular cartilage and chondrocytes produce hemopoietic colony-stimulating factors in culture in response to IL-1. J Immunol 147: 1238–1246
Leizer T et al. (1990) Cytokine regulation of colony-stimulating factor production in cultured human synovial fibroblasts: I. Induction of GM-CSF and G-CSF production by interleukin-1 and tumor necrosis factor. Blood 76: 1989–1996
Lawlor KE et al. (2004) Critical role for granulocyte colony-stimulating factor in inflammatory arthritis. Proc Natl Acad Sci USA 101: 11398–11403
Burlak C et al. (2006) Maturation of human neutrophil phagosomes includes incorporation of molecular chaperones and endoplasmic reticulum quality control machinery. Mol Cell Proteomics 5: 620–634
Lominadze G et al. (2005) Proteomic analysis of human neutrophil granules. Mol Cell Proteomics 4: 1503–1521
Opdenakker G et al. (2001) Gelatinase B functions as regulator and effector in leukocyte biology. J Leukoc Biol 69: 851–859
Acknowledgements
The authors' research is supported by the Reid Charitable Trusts, the Arthritis Foundation of Australia, the Cancer Council of Australia and the National Health and Medical Research Council of Australia.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
IP Wicks and JL Eyles are collaborating on the commercial development of G-CSF antagonists. JL Eyes and IP Wicks have declared associations with the following companies/organizations: ABC, CDE, FGH, Murigen Therapeutics and Zenyth Therapeutics. AW Roberts and D Metcalf have declared they have no competing interests.
Rights and permissions
About this article
Cite this article
Eyles, J., Roberts, A., Metcalf, D. et al. Granulocyte colony-stimulating factor and neutrophils—forgotten mediators of inflammatory disease. Nat Rev Rheumatol 2, 500–510 (2006). https://doi.org/10.1038/ncprheum0291
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1038/ncprheum0291
This article is cited by
-
Tenosynovial giant cell tumor: a case report
Journal of Medical Case Reports (2023)
-
LRG1: an emerging player in disease pathogenesis
Journal of Biomedical Science (2022)
-
Neutrophilic Dermatosis and Management Strategies for the Inpatient Dermatologist
Current Dermatology Reports (2022)
-
Mammary tumour cells remodel the bone marrow vascular microenvironment to support metastasis
Nature Communications (2021)
-
Neutrophil-derived granule cargoes: paving the way for tumor growth and progression
Cancer and Metastasis Reviews (2021)